Dysbiosis and Depression: Understanding the Gut-Brain Connection

Have you ever had a “gut feeling” that something was off – not just in your belly, but in your mind, too? As it turns out, that intuitive connection between the gut and the brain is more than a metaphor. It’s science.
Over the past decade, researchers have uncovered a fascinating link between our digestive health and our mental well-being. This is more than just a trend or buzzword. It’s a powerful insight into how the microbial world inside us. Known as the gut microbiome, this system in our body may play a key role in mood disorders like depression and anxiety.
Let’s explore how gut imbalance, or dysbiosis, can impact your mental health and what you can do about it.
The Gut: More Than Just Digestion
The gut does far more than break down food. It houses over 100 trillion microbes like bacteria, fungi, and viruses. All these help digest nutrients, support the immune system, and even produce neurotransmitters like serotonin. In fact, nearly 90% of the body’s serotonin is made in the gut, not the brain.
When balanced, this ecosystem of microorganisms keeps things running smoothly. But when that balance is thrown off by stress, diet, antibiotics, or chronic illness, it can lead to dysbiosis. That’s when the gut’s “bad” bacteria outnumber the beneficial ones. This then sets off a chain reaction that can disrupt everything from digestion to mood regulation.
How Dysbiosis Affects the Brain
So, how exactly does a bacterial imbalance in your gut lead to emotional distress?
It all comes down to the gut-brain axis. This is the communication superhighway that connects the gastrointestinal system with the central nervous system. When dysbiosis occurs, it can cause inflammation in the gut lining—a condition often referred to as “leaky gut.” This inflammation sends distress signals to the brain that increases the production of stress hormones like cortisol and contributes to neuroinflammation.
This, in turn, can interfere with mood, cognition, and emotional regulation. People with dysbiosis often report feeling more anxious, fatigued, irritable, and emotionally flat. While depression has many causes, there’s growing evidence that gut health could be a major contributing factor.
In other words, if your gut is unhappy, your mind might be too.
What the Research Says
Science is beginning to catch up to what many integrative doctors have long suspected: the microbiome matters.
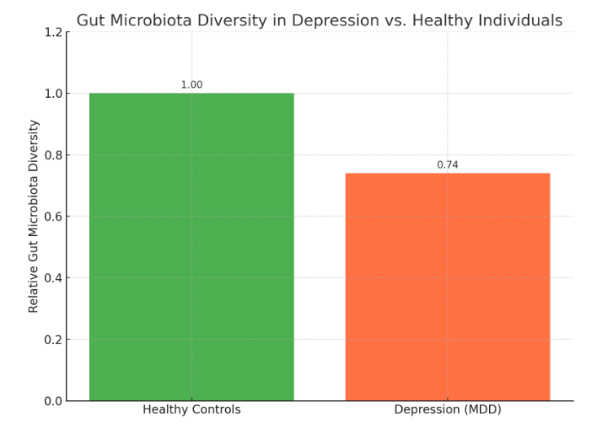
One large-scale study found that people with major depressive disorder had significantly less microbial diversity in their gut compared to healthy individuals. Researchers identified certain beneficial strains, like Bifidobacterium and Lactobacillus, that were consistently low in those with depression.
Animal studies back this up, too. Mice given antibiotics to disrupt their gut microbiota showed increased anxiety-like behaviors. Interestingly, when their microbiota was restored through probiotic supplementation, their symptoms improved.
The Role of Inflammation
One key culprit in this gut-brain dynamic is inflammation. When the gut is imbalanced, it can become a breeding ground for inflammatory cytokines. These are the chemical messengers that travel through the bloodstream and can cross the blood-brain barrier.
Once in the brain, these inflammatory signals may alter neurotransmitter activity. They can affect serotonin and dopamine production, both of which play crucial roles in regulating mood. This inflammation-based model of depression offers a different way of understanding the condition. We can begin looking at it not simply as a “chemical imbalance” in the brain, but as a systemic issue rooted, at least in part, in the gut.
Food, Mood, and Mental Health
It’s no surprise, then, that what you eat has a direct impact on how you feel. Diets high in processed foods, refined sugars, and unhealthy fats can fuel dysbiosis and inflammation. Meanwhile, diets rich in fiber, fermented foods, and whole, plant-based ingredients support microbial diversity.
Many patients notice dramatic shifts in mood and energy once they begin eating to support their gut. It’s not magic—it’s microbiome science. Foods like kimchi, sauerkraut, yogurt, and fiber-rich vegetables feed the good bacteria. As a result, they promote a healthier gut lining and, by extension, a healthier mind.
What Can You Do to Support Your Gut-Brain Connection?
If you’re struggling with depression, it’s worth considering your gut health as part of the bigger picture. Healing the gut won’t necessarily replace therapy or medication. But it can be a powerful complement to a comprehensive mental health plan.
Functional medicine takes a whole-body approach. Practitioners may use stool testing to assess your microbiome, blood work to evaluate inflammation levels, and dietary or lifestyle strategies to bring your gut back into balance.
Here are a few simple steps you can take to begin healing your gut:
- Start by reducing your intake of ultra-processed foods, added sugars, and artificial additives. These disrupt the microbiome and promote inflammation.
- Focus on nutrient-dense, whole foods, especially those rich in prebiotic fibers, like asparagus, oats, and garlic.
- Adding fermented foods like kefir, kimchi, or miso can introduce beneficial bacteria.
- Taking high-quality probiotic supplements may help restore microbial balance.
Finally, don’t overlook the impact of stress. Chronic stress can compromise the gut lining and reduce beneficial bacteria. Practicing stress-reduction techniques like mindfulness, yoga, or regular movement is key.
A Brighter Path Forward
Depression is complex, and healing it requires more than a one-size-fits-all solution. But the growing research into the gut-brain connection offers a hopeful, empowering message:
Your mental health isn’t just in your head—it’s in your gut, too.
If you’ve tried traditional approaches and still feel like something’s missing, it may be time to look deeper. Supporting your gut may be the missing link in your path to feeling like yourself again.
At Mind Body 7, we understand the importance of treating the whole person. Our integrative team combines psychiatry, psychotherapy, and functional medicine to help uncover the root causes of your mental health symptoms. After all, you deserve more than symptom management. You deserve true healing.
Ready to explore how your gut health could be affecting your mood? Let’s start that conversation together.
Word play!
- I’m your second brain, and I live in your belly. What am I?
Clue: 9 letters, starts with “m”
Answer: microbiome
- I’m the fancy word for when your gut bugs go bad.
Clue: Starts with “d,” ends with “sis”
Answer: Dysbiosis
- I’m the body’s alarm system that can get stuck in “on” mode.
Clue: 11 letters, starts with “i”
Answer: Inflammation
Cited Research Articles
Perturbations in Gut Microbiota Composition in Psychiatric Disorders: A Review and Meta-Analysis. Nikolova VL, Smith MRB, Hall LJ, et al. JAMA Psychiatry. 2021;78(12):1343-1354. doi:10.1001/jamapsychiatry.2021.2573.
The Gut Microbiota and Depressive Symptoms Across Ethnic Groups. Bosch JA, Nieuwdorp M, Zwinderman AH, et al. Nature Communications. 2022;13(1):7129. doi:10.1038/s41467-022-34504-1.






